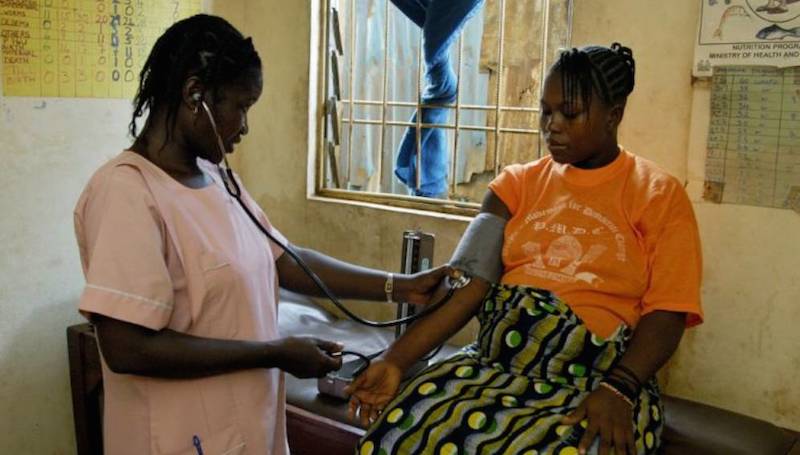
With progress on eradicating malaria slowing down in 2018 according to the World Health Organisation, a new research by medical experts has found there is an urgent need to review a key medication administered to pregnant women, particularly in areas of established anti-malarial drug resistance.
According to the 2018 World Malaria report, five countries accounted for nearly half of all malaria cases worldwide, and Nigeria accounted for 25 percent of this, making it even more important that policy makers in the country take steps to address this new concern.
A global team of researchers, led by a team at the Liverpool School of Tropical Medicine (LSTM), are calling for a review of drug-based strategies used to prevent malaria infections in pregnant women, in areas where there is widespread resistance to existing anti-malarial medicines.
Feikoter┬ĀKuile, a professor and expert in malaria in pregnancy, recently worked with a multi-disciplinary team including the US Centres for Disease Control and Prevention, the World Wide Anti-malarial Resistance Network (WWARN) and Duke University to complete the most comprehensive study to date of the impact of Sulphadoxine-Pyrimethamine (SP) drug resistance on the effectiveness of intermittent preventative treatment (IPTp).
Published this week in Lancet Infectious Diseases, the results demonstrate that the clinical effectiveness of SP in protection of pregnant women against malaria is compromised in certain areas.┬Ā┬ĀThe experts urgently call for further investigation into alternative strategies or drugs to prepare for further growing resistance to this mainstay of preventive therapy.
The WHO recommends intermittent preventive treatment (IPTp) in malaria endemic areas. The only anti-malarial currently recommended for IPTp is SP; to date IPTp with SP has effectively resulted in reductions in maternal anaemia, low birth weight and neonatal mortality. However, with the growing threat of drug resistance emerging or spreading in sub-Saharan Africa, this protection is now at risk.
It is estimated that without protection during pregnancy, 45 per cent of 32 million pregnancies in malaria endemic sub-Saharan Africa are exposed to Plasmodium falciparum malaria, leading to 900,000 malaria-associated low birth-weight deliveries. Low birth weight, anaemia and other serious adverse birth outcomes result in numerous longer-term health issues for infants.
According to┬ĀKuile, more than 100,000 birth outcomes across Sub-Saharan Africa were reviewed, and results suggest that the widely used anti-malarial SP for preventive therapy remains very effective in many parts of Africa, but that there is a clear trend toward reduced effectiveness with increasing levels of resistance by the malaria parasite to SP.
In some areas where highest grade of resistance was observed, the effectiveness of SP appears to be fully compromised. According to the research, this indicates alternative approaches to the prevention of malaria in pregnancy are urgently needed to achieve better birth outcomes for pregnant women.
Anna Maria van Eijk, first author of the published research, called for further analysis into the potential additional benefits that SP may continue to have even in areas where it is no longer able to kill malaria parasites. For example, through its anti-microbial effects, or perhaps SP has some anti-inflammatory and immune modulating effects that are similar to those discovered for widely used antibiotic cotrimoxazole.
This is important as SP may not work as well as other anti-malarials in high SP resistance areas, but it may still be able to help reduce poor birth outcomes, such as low birth weight through these other mechanisms.
ŌĆ£This large-scale analysis has given us a powerful message: the increasing prevalence of molecular markers of SP is correlated with a decrease in effectiveness of SP to reduce low birth weight and malaria infections,ŌĆØ noted Carol Sibley, WWARNŌĆÖs Senior Scientific Advisor from the University of Washington.
It is recommended that molecular monitoring of parasites in humans is a valuable tool for policy makers to monitor the spread of anti-malarial resistance, and assess its impact as a prevention strategy for malaria in pregnancy, and the resulting effects.
CALEB OJEWALE
┬Ā
┬Ā