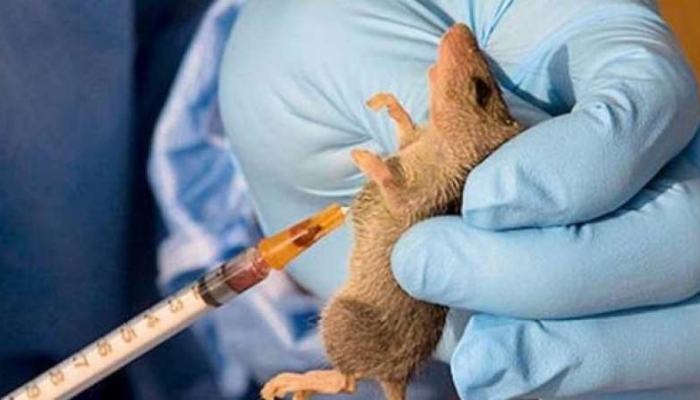
Since its first discovery in the town of Lassa, Borno State, in 1969, Lassa fever has transitioned from a localised medical curiosity to a permanent national health threat. 57 years later, the disease remains entrenched in Nigeria, with recent data showing a worrying surge in both geographic spread and lethality.
According to the Nigeria Centre for Disease Control (NCDC), the country has recorded Lassa fever outbreaks in 49 of the 57 years since its discovery, representing an 86 percent occurrence of the time. The current situation is particularly grim.
Between late 2025 and early 2026, the Case Fatality Rate (CFR) jumped to 22 percent, up from 16 percent in 2024. In a seven-week window, 318 cases were confirmed out of 1,469 suspected infections, resulting in 70 deaths. The virus continues to claim frontline workers nationwide, with 15 of them battling healthcare infections in the latest cycle.
Read also:┬ĀLassa fever deaths rise to 75 as fatality rate climbs to 23%
The Diagnostic Trap
One of the primary reasons Lassa fever remains so deadly is the ŌĆ£Late PresentationŌĆØ phenomenon. According to the World Health Organisation (WHO), the symptoms of Lassa feverŌĆöfever, headache, and general malaiseŌĆöare indistinguishable from malaria or typhoid in the early stages.
Experts like Akolade Jimoh note that many patients spend critical days treating the wrong illness. By the time uncontrollable vomiting, swelling, or haemorrhaging begins, the viral load is often too high for effective intervention.
A massive financial barrier compounds this delay. Joseph Okoeguale, director at the Lassa Fever Research Institute, currently known as the Institute of Viral and Emergent Pathogens Control and Research in Edo State, also highlighted poor access to diagnostic kits and high treatment costs.
ŌĆ£Early diagnosis significantly improves survival chances, but access to testing and high treatment costs remain limited in many affected areas,ŌĆØ he noted.
ŌĆ£A single diagnosis costs about N250,000, an amount too expensive for many Nigerians in rural communities where the disease is prevalent,ŌĆØ Okoeguale added.
The biological ŌĆ£engineŌĆØ of the disease is the Mastomys natalensis (multimammate rat). These rodents live in proximity to humans in rural areas, shedding the virus in their urine and faeces.
Humans are infected through direct contact with these excretions, touching contaminated objects, or eating food ŌĆ£visitedŌĆØ by the rats.
ŌĆ£We have recorded higher cases in rural communities and some urban areas with poor hygiene conditions,ŌĆØ Okoeguale noted.
While Edo and Plateau states remain hotspots according to NCDC data, the virus is migrating. Bayelsa, which had no recorded cases for over 50 years, reported its first fatality in 2023, a 42-year old civil servant who died from the disease, signalling that no region is safe.
Read also:┬ĀBenue ramps up surveillance to contain Lassa fever as cases surge
Stories of survivors
In 2023, Mtsenem Jacob, a surgical nurse at Benue State University Teaching Hospital (BSUTH) and survivor, recounted how he battled the virus while on night duty.
After several days of unsuccessful malaria and typhoid treatment, he opted for a Lassa fever test. ŌĆ£I quickly ran Lassa fever tests as soon as I discovered that malaria and typhoid treatments were not effective,ŌĆØ Jacob said.
Ikenna Chibuike, another survivor from Ebonyi State, highlighted how he started treatment for malaria and typhoid when the symptoms started.
ŌĆ£ I started treating malaria and typhoid without progress until I started stooling and vomiting uncontrollably, before being diagnosed with Lassa fever,ŌĆØ Chibuike noted.
Experts note that when malaria and typhoid treatment becomes ineffective, patients should immediately be tested for Lassa fever, and treatment must commence within the early stage of the disease presentation.
Barriers to Lassa fever eradication
High rodent reservoir, poor hygiene, high treatment cost, poor access to diagnostic kits, poor research funding and lack of vaccine or drugs that have undergone clinical trial are some of the major barriers to eradicating Lassa fever in Nigeria.
ŌĆ£There is no specific treatment for Lassa fever,ŌĆØ noted Ephraim Ogbaini-Emovo, director at Lassa Fever Research Institute. Experts say that the current drug (Rivabirin) used has not undergone a clinical trial for the treatment of the disease, and sometimes has side effects like anaemia and hearing loss.
ŌĆ£It is difficult to eradicate or curb the spread of the disease due to poor hygiene, as improperly stored foods and bushy environments are risk factors for contracting the disease,ŌĆØ Okoeguale noted. However, good hygiene, like storage of staple goods like rice, beans and garri, is a major barrier to curbing the spread of the disease.
ŌĆ£Lassa fever is still very much under-diagnosed because the facilities are not available in many parts of the country and treatment is not cheap,ŌĆØ he added.
WhatŌĆÖs the way out?
Accelerating vaccine development, strengthening cross-border collaboration between Nigeria and other countries, as well as increasing investment in research, diagnostics, treatment, and culturally responsive interventions, are major strategies for eradicating the disease.
ŌĆ£Cultural practices such as burial rites, food storage and handling often expose people to the disease, and it is important to improve on these through awareness campaigns,ŌĆØ Jimoh noted.
Surveillance centres on early case detection through community reporting and laboratory confirmation, alongside strict infection prevention measures such as personal protective equipment (PPE) use, patient isolation, safe burials, improved sanitation, rodent-proof food storage, and sustained public awareness on hygiene and rodent avoidance.
Read also:┬ĀLassa fever deaths reach 70 amid rising infections among health workers
ŌĆ£We must ensure to clear surrounding bushes, invest in vaccine development and engage in enlightenment campaigns to eradicate the disease,ŌĆØ Okoeguale noted.
Although Lassa fever is prevalent in other West African countries like Guinea, Sierra Leone, Cote dŌĆÖivoire, Burkina Faso, Liberia, Guinea and parts of Benin, none of these countries have been able to eradicate the disease as at the time of this report.
ŌĆ£Only Sierra Leone has stronger case management systems and improved diagnosis and early detection labs,ŌĆØ Jimoh noted.