Nigeria’s public health response has increasingly begun to resemble what Charles Dickens once described as a Tale of Two Cities, where two realities exist within the same nation but are governed by different priorities. One Nigeria mobilises swiftly, deploys resources, communicates clearly, and defeats disease with remarkable efficiency. The other Nigeria watches helplessly as preventable illnesses claim lives year after year, particularly among ordinary citizens and frontline health workers.
The difference between both realities is simple: who is at risk.
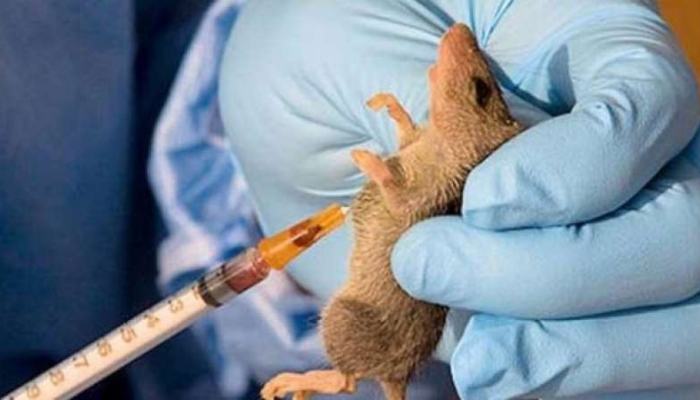
When diseases threaten political leaders, business elites, diplomats, and urban centres of influence, Nigeria suddenly discovers urgency, coordination, and competence. But when outbreaks remain largely confined to rural communities, poor households, and overstretched public hospitals, response mechanisms slow to a familiar crawl. The ongoing Lassa fever outbreak painfully exposes this contradiction.
According to the Nigeria Centre for Disease Control (NCDC), at least 70 Nigerians have already died in the current outbreak, with infections rising alarmingly among healthcare workers. Confirmed cases jumped significantly within weeks, spreading across multiple states like Ondo, Bauchi, Taraba, Edo, and Benue. Even more troubling is the case fatality rate, now exceeding previous records.
Yet, despite the recurring nature of Lassa fever in Nigeria, the nation continues to respond as though confronted with a surprise enemy each year.
Nigeria has demonstrated before that it possesses the capacity to defeat deadly outbreaks. During the 2014 Ebola crisis, decisive leadership, aggressive contact tracing, public communication, and coordinated emergency action helped Nigeria halt what could have become a continental catastrophe, and the world applauded Nigeria’s response.
Similarly, during the COVID-19 pandemic, emergency structures were activated almost overnight. Isolation centres emerged, funding flowed rapidly, testing capacity expanded, and daily national briefings became routine. Airports were monitored, movement restricted, and political attention remained unwavering.
This was because Ebola and COVID-19 threatened everyone, including the elite. Air travel, diplomatic interaction, and urban transmission meant that no social class was insulated. Decision makers suddenly understood that failure carried personal risk. But today, the Lassa fever case, however, tells a different story.
Lassa fever is not new, as Nigeria has battled it for over five decades since it was first identified in 1969. Unlike Ebola, its transmission is closely linked to poverty conditions (overcrowded housing, poor sanitation, food storage practices, and rodent infestation). The disease thrives where infrastructure fails in rural settlements, underserved communities, and poorly funded hospitals.
The tragedy is that, because Lassa fever disproportionately affects populations far removed from political power, national urgency fades after each outbreak headline. The response becomes seasonal rather than systemic, as hospitals lack infection prevention equipment, healthcare workers remain inadequately protected, and diagnosis is delayed because suspicion levels remain low.
The result of this becomes predictable, as doctors and nurses, already scarce, become victims themselves. The sad aspect is that a nation that cannot protect its healthcare workers is effectively dismantling its own defence system.
Nigeria’s continued struggle becomes even more embarrassing when compared with how other nations have handled endemic infectious diseases.
Nations such as Sierra Leone and Liberia, devastated by Ebola less than a decade ago, invested heavily in community surveillance, laboratory networks, and infection control training afterward. Rwanda strengthened its disease surveillance architecture despite limited resources, prioritising early detection and community health education.
Even nations confronting recurring haemorrhagic fevers have shifted from emergency reaction to permanent preparedness.
By contrast, Nigeria still activates emergency response mechanisms almost yearly for Lassa fever, treating recurrence as inevitable rather than a policy failure.
The implications of this attitude extend far beyond mortality figures, as this is the erosion of healthcare confidence. When hospitals become infection centres, patients delay seeking treatment, worsening transmission and fatalities.
Also, there is economic loss, as outbreaks disrupt agriculture, trade, schooling, and workforce productivity in affected states, which quietly drains local economies.
Likewise, professional migration occurs as healthcare workers facing repeated exposure without adequate protection increasingly choose to leave Nigeria. The ongoing brain drain within the medical sector is partly fuelled by unsafe working conditions.
Similarly, there is reputational damage. A nation aspiring to regional leadership cannot remain unable to control an endemic disease it has studied for decades.
Nigeria’s Lassa fever challenge is no longer primarily scientific. The virus is understood, preventive measures are known, and treatment protocols exist, but the problem is the lack of the right governance policy.
Public health investment remains reactive instead of preventive, as environmental sanitation campaigns are occasional. Primary healthcare systems, the first line of outbreak detection, remain weak across many local governments. More fundamentally, disease control has not been institutionalised as national security policy.
Until epidemic diseases affecting rural Nigerians are treated with the same seriousness as threats reaching Abuja or Lagos high society, outbreaks will persist.
Governors and local government authorities must be held accountable for preparedness indicators, just as economic performance is measured.
Ultimately, Lassa fever exposes more than a health crisis; it reveals a moral dilemma.
Does the Nigerian state value all lives equally? If the answer is yes, then recurring deaths from a preventable and well-understood disease represent national failure. If the answer is no, then Nigeria risks institutionalising a dangerous hierarchy of survival, where response intensity depends on social status.
Diseases do not permanently respect class boundaries. Today’s rural outbreak can become tomorrow’s urban emergency.
Nigeria proved during Ebola and COVID-19 that victory against deadly diseases is possible when leadership acts decisively. The shame is not ignorance or lack of capacity. The shame is selective urgency.
Until Nigeria fights Lassa fever with the same determination reserved for diseases that threaten the elite, the country will continue to mourn avoidable deaths, year after year, from an enemy it already knows how to defeat.