ŌĆ”Nigeria has an average bed capacity of 0.25 beds per 1000 persons.
Shot in the head by armed men around 5:00am at his residence, Osaze Daniel (not his real name) was rushed to a nearby general hospital at Sango Ota, only for his family to discover there were no vacant beds.
They desperately searched for other hospitals but found none. Attempting to transfer him to Lagos, he died on the way.
ŌĆ£We went to four different hospitals, but they all said there was no bed to admit him. We finally decided to take him to Lagos, but he never made it,ŌĆØ an eyewitness told this reporter.
In another case, a cancer patient recounted on social media how she repeatedly sat in a corridor for hours, sometimes in rainfall, just to see her doctor at the Federal Medical Centre, Jabi, Abuja.
Read also:┬ĀNigerians deserve world-class healthcare at home ŌĆō Dr Onyia
She said the porter often had to search the entire facility for a vacant bed before she could receive chemotherapy.
ŌĆ£I canŌĆÖt tell you how many times I had to sit outside in the corridor- even when it rained ŌĆō just to see my doctor on clinic days,ŌĆØ she wrote.
ŌĆ£Until a few months ago, there was no designated ward for chemotherapy. The porter always had to look for beds before we could be taken in for treatment.ŌĆØ
These stories underscore the urgent need to upgrade NigeriaŌĆÖs public healthcare facilities, experts say.
Fewer beds, more patients
Martin Uche, a health analyst, highlighted that Nigeria as a whole has fewer than 10,000 beds in 40,000 public health facilities.
ŌĆ£For a population of nearly 230 million people, this is catastrophic in the case of a pandemic,ŌĆØ another source stated.
Only about eight percent of over 40,000 registered health facilities across the country have substantial inpatient bed capacity that meets global standards, according to recent 2025 reports by Fortren and Company.
This has resulted in a critically low national bed-to-patient ratio. Nigeria currently has 0.25 beds per 1,000 people, far below AfricaŌĆÖs average of one bed per 1,000 and the global average of 2.7 beds, according to the World Health Organization (WHO).
ŌĆ£Despite over 40,000 facilities, only eight percent have inpatient beds, resulting in a globally low bed to patient ratio of just 0.25 beds per 1,000 people,ŌĆØ the Fortren and Company 2025 report noted.
ŌĆ£As a result, patients are bounced from facility to facility, referrals overwhelm the system, and delays in treatment often prove fatal,ŌĆØ the report stated.
Read also:┬ĀPresidency tasks states to scale up domestic financing for healthcare
Emmanuel Osemudiame, co-founder and chief executive of Salvus Emergency, described the situation as alarming, citing a databank of 10,000 health facilities by its company.
ŌĆ£Looking at international standards, only a few hospitals in Nigeria come close,ŌĆØ he said. ŌĆ£Most public hospitals simply do not have enough beds,ŌĆØ he stated.
A source also revealed that Lagos University Teaching Hospital (LUTH) has about 3,000 beds.
ŌĆ£A hospital as large as LUTH should have between 5,000 and 10,000 beds,ŌĆØ the source said.

Treatment on benches
Another source shared how some emergency patients at the University College Hospital (UCH), Ibadan, were treated on benches due to inadequate beds, noting that the ICU had only 20 beds and many patients were turned away.
ŌĆ£My heart broke when I visited the UCH and saw patients being turned back for lack of beds. The only patient admitted at the time I visited was placed on a bench after much pleading by family members,ŌĆØ the source said.
Osemudiame noted that delayed care makes treatment more expensive. ŌĆ£By the time patients end up on benches, complications have already set in, and complications raise treatment costs,ŌĆØ he said.
Solomon Damien, a medical expert, also highlighted the impossible decisions health workers face daily.
ŌĆ£ItŌĆÖs a critical situation. Sometimes we have to make tough choices about who gets a bed and who doesnŌĆÖt, depending on how severe the cases are,ŌĆØ he said.
Read also:┬ĀUNICEF urges media to lead health enlightenment efforts in rural communities
Reasons for inpatient bed shortages
Experts attribute NigeriaŌĆÖs inpatient bed shortages to several systemic failures, including poor information flow, an overreliance on small and poorly equipped outpatient facilities, inadequate bed allocation to hospitals by stakeholders, weak policy implementation, and widespread fragmentation across the health system.
ŌĆ£There is no real-time dissemination of information in many public or tertiary hospitals,ŌĆØ Osemudiame explained.
ŌĆ£A consultant may discharge a patient, but nurses remain unaware because patients often delay before leaving the facility,ŌĆØ he added.
According to him, this communication gap leads to situations where beds appear unavailable even when they should be vacant.
Experts also note that Nigeria has too many small, disaggregated outpatient facilities that are poorly equipped.
ŌĆ£Fortren and Company reports that during peak malaria seasons, 70 percent of these rural northern facilities turn away patients due to bed shortages,ŌĆØ the report stated.
Osemudiame added that the licensing of unqualified or inadequately equipped health facilities by regulatory bodies worsens the crisis and enables quackery.
ŌĆ£Some so-called specialist hospitals have only six beds in the entire facility,ŌĆØ he said.
ŌĆ£Many of these small, licensed facilities are not qualified to deliver the services they claim to handle. When patients are referred to them, they are turned back because there are simply no beds,ŌĆØ he added.
ŌĆ£That is why you often hear patients say they visited several hospitals and were rejected due to lack of bed space,ŌĆØ Osemudiame explained.
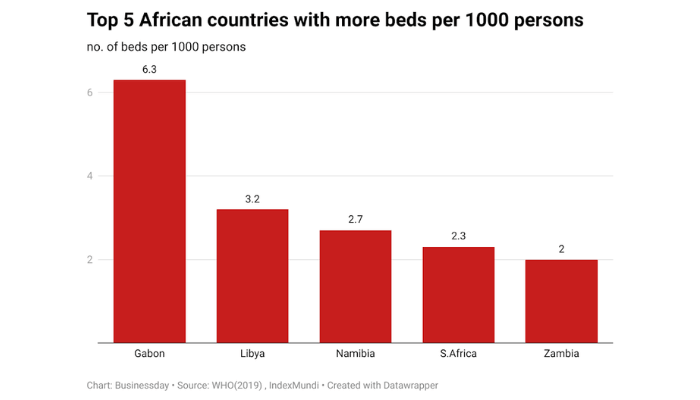
Global outlook
Across Africa, bed capacity varies widely. Gabon leads with 6.3 beds per 1,000 people, followed by Libya (3.2), Namibia (2.7), South Africa (2.3) and Zambia (2.0), according to WHO (2018) and IndexMundi. At the lower end, Mali has just 0.1 beds per 1,000 people.
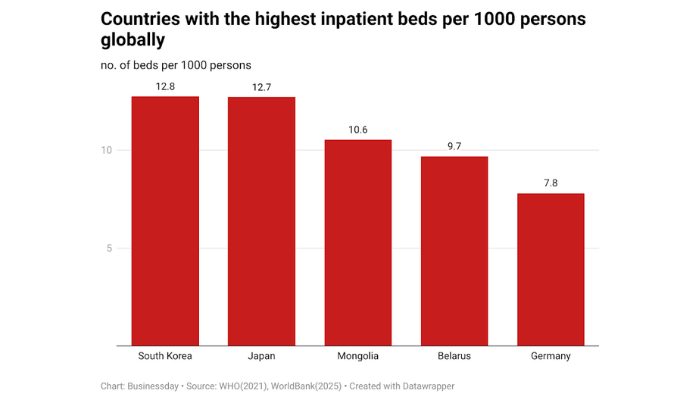
Globally, South Korea (12.75) and Japan (12.72) had the highest bed capacity in 2021, based on the WHO data.
More striking is the comparison between Saudi Arabia, with a population of 32 million and 2.43 beds per 1,000, and Nigeria, with 230 million people but only 0.25 beds per 1,000.
Experts say this gap highlights the urgent need for large-scale investment and structural reforms in NigeriaŌĆÖs healthcare system.
Read also:┬Ā├Æbß║╣╠Ć Il├Ī ati Omi At├Ī (Okra sauce): Proudly Nigerian healthy superfood that can gain UN cultural status
What can be done?
Experts have called for stronger cohesion across NigeriaŌĆÖs healthcare system in order to enable seamless communication across all healthcare facilities in the country. They also emphasise that resources should prioritise equipping existing hospitals with more inpatient beds, rather than building new facilities. In addition, they stressed the need to streamline licensing processes, enforce global standards before facilities are approved, and adopt technology to solve real-time operational gaps, especially during emergencies.
ŌĆ£NigeriaŌĆÖs health systems need to be unified in the sense that all public health facilities nationwide can be connected on a digital platform to enable the sharing of information in real time, so that whenever thereŌĆÖs an emergency, you can easily access information from each other,ŌĆØ Osemudiame noted.











